Course:FNH200/Lessons/Lesson 12/Page 12.6
12.6 Examples of Natural Contaminant as Toxicants
Mycotoxins
Mycotoxins are substances produced by moulds, which may be toxic. Mycotoxins may occur by direct contamination (due to mould growth on the food) or by indirect contamination (by using a food ingredient that was contaminated). Mycotoxins can be highly toxic to the body, some have been known to cause cancer in animal tests, others are mutagenic and able to cause mutation, and others are teratogenic and capable of causing deformities in embryos. Mycotoxins are invisible to the eye, are often unchanged by heat and can potentially spread throughout a product. As a result, any sign of visible mould could indicate that the product contains mycotoxins and should be thrown away.
| Want to learn more? |
|
Of the many known mycotoxins (aflatoxins, sterigmatocystin, ochratoxin A, citrinin and patulin), the aflatoxins are of greatest concern because they are potent liver toxins in all animals in which they have been tested and carcinogens in some species. The different aflatoxins (B1, B2, G1, G2, M1and M2) may be found in various commodities including peanuts, corn, wheat, rice, cottonseed, copra, nuts, milk, eggs, and cheese.
One additional comment needs to be made in connection with the regulation of mycotoxins. Aflatoxins are not directly regulated in The Food and Drugs Act. In Canada, this has caused some problems in the past. A challenge of the contention that aflatoxin was injurious to human health caused a court to dismiss a charge of selling contaminated peanut butter that contained greater than 20 ppb of aflatoxin. To get around that problem, the act and regulations were changed to state that peanut butter would be considered contaminated, and therefore not fit for sale, if it contained aflatoxins in excess of 15 ppb.
Generally, any food which contains mould should be thrown out however because the risk of mycotoxins is fairly low in some instances, the benefit of saving the product may outweigh the potential risks involved.
The following should be considered when we encounter a mouldy food:
- Was the food refrigerated? Did the mould grow on the product while it was refrigerated? If it has, it is likely that the product does not contain aflatoxins (these are not normally produced under refrigerated conditions).
- The amount of mould on the product should also be considered, for example, if there is a tiny green mould colony on a large block of cheese, the benefits of cutting that portion off (about 2.5 cm around and beneath the cheese) are much greater than the risks involved, especially relative to the benefits of trimming extensive mould growth on a tiny piece of cheese.
- The type of food the mould is growing on should also be considered; “trimming” mould should not be done on soft, semi-solid, or liquid foods, or foods likes jams/jellies and baked products. In these products, the ability for the mould toxins to spread (via the mould mycelia) are much greater. In these cases, the risks outweigh the benefits of saving the product.
- To ensure that mould growth does not occur at home, consumers can try to prevent mould growth by minimizing contact of food with air as well as package (wrap) and refrigerate products appropriately.
| Critical Thinking |
|
Bacterial Toxins
The two most important bacterial toxins are those produced by Clostridium botulinum and Staphylococcus aureus, which are ubiquitous microorganisms in our environment. Food poisoning caused by these two types of bacteria can be considered as due to food intoxications, because it is the chemical toxin produced by the bacteria, as opposed to the bacteria themselves (in the case of foodborne infections), that produces the toxicity. The toxins can produce illness even if the bacteria producing them have been killed. We will explore these in further detail later in this lesson (under "foodborne diseases").
Check out the recent Health Hazard Alerts regarding possible Clostridium botulinum contamination.
http://www.inspection.gc.ca/about-the-cfia/newsroom/food-recall-warnings/complete-listing/2019-03-15/eng/1552702897100/1552702899415
Seafood Toxins
Most of the natural toxicants that we encounter in our food supply are in products of plant origin. Animal tissues are much less frequently contaminated with natural toxicants. Part of the reason for this might be the fact that animals are very similar in their make-up and metabolism to humans. Animals would react similarly to toxins in their environment as humans and consequently we are not confronted with animal tissues that are from diseased or poisoned animals. For this reason, while it is a somewhat broad generalization, most natural toxicants in foods categorized as animal origin are found in seafoods rather than other animal products, and in fact, in many of these cases, the source of the toxicants originate from marine algae or through the action of microorganisms.
There are many types of seafood toxins; here we will review some of the most common ones: Histamine, Saxitoxin, Domoic acid, and Tetrodotoxin.
Histamine
Poisoning is known to result from eating scombroid fishes, i.e. fish of the Scombrida and Scomberesocidae families, including tuna, bonito and mackerel. The poisoning results in nausea, vomiting, facial flushing, headache, epigastric pain, thirst, itching of the skin and hives. The effects usually subside within 12 hours but in some severe cases death has resulted.
Scombroid poisoning is due to an allergic-type reaction to high levels of histamine or a histamine-like substance. Histidine, a naturally occurring amino acid which is particularly high in scombroid fish, is converted to histamine by bacterial action on the dead flesh of the fish. Histamine has strong vaso-active properties and in sufficient quantities will cause blood pressure changes resulting in symptoms as indicated above. It should be noted that toxic amounts of histamine may be formed before the fish starts to smell or taste bad ("spoil"). Histamine formation is dependent on the holding time and temperature of the fish during transportation and storage.
It is also important to note that histamine and other vaso-active amines may be found in many fermented foods such as cheese, wine and pickled herring.
Saxitoxin
Saxitoxin and a group of 18-24 marine biotoxins derived from saxitoxin are thought to be responsible for the condition known as paralytic shellfish poisoning (PSP). This condition is the result of consuming shellfish, such as mussels, oysters, and clams, containing the toxin. The toxins can also accumulate in the liver of crustaceans such as crabs and lobsters.
The toxin is ineffective against the shellfish, which are able to absorb the toxin, concentrate it in their tissues and pass it onto the species feeding on them (in this case, humans).
Symptoms of saxitoxin include: tingling in the mouth, lips and finger tips. Sight and hearing are modified in much the same way as caused by alcohol intoxication. Speech becomes incoherent.
Saxitoxin is a contaminant which the shellfish consume as part of their occasional food supply. The shellfish feed on a variety of microscopic plankton among which are certain toxic dinoflagellates. At certain times of the year, under certain conditions, these dinoflagellates increase greatly in number and concentration in the oceans. This is often referred to as a bloom or "red tide."
During periods of bloom or red tide, the shellfish are exposed to and concentrate large amounts of saxitoxin. Saxitoxin is extremely stable and takes a long time to be flushed from the tissues of the shellfish. It is for this reason that during red tide season and for a considerable time afterwards, harvesting of shellfish is prohibited.
Saxitoxin is considered one of the potent toxins, the minimum lethal dose being about 1.0-4.0 mg/kg of body weight. However, because of the variability in the concentration of toxin in the shellfish, it is very difficult to indicate a maximum amount of shellfish tissue that can be consumed. This is obviously a situation which is not at all hazardous to anyone who rarely harvests and consumes shellfish. However the hazard increases significantly, for those who are uninformed and are fond of shellfish, particularly those harvested in areas known to be subject to red tide situations.
Domoic Acid
Domoic acid is (an analog of the amino acid glutamic acid), is found in some marine algae (dinoflagellate Nitschia), which can accumulate in filter feeding shellfish such as clams, mussels, scallops and oysters. Consumption of shellfish with this naturally occurring marine biotoxin can lead to amnesic shellfish poisoning (ASP).
Domoic acid, a neurotoxin, is capable of causing lesions in the central nervous system. It was first discovered in 1987 in Canada, when an outbreak occurred in individuals consuming mussels in Prince Edward Island. Of 107 individuals who were affected, four died. Most experienced gastroenteritis, and many older persons, or others with underlying chronic illnesses, developed neurological symptoms including memory loss. In this case, enough toxin was absorbed through the gastrointestinal system to cause the effects. The most severely affected cases still had significant memory loss five years after the incident.
Routine testing for the toxin is conducted, and areas in which the toxin occurs in the shellfish are closed to harvesting. Thus, the risk of amnesic shellfish poisoning is high only for individuals who choose to ignore signs indicating closure of areas to shellfish harvesting.
If you regularly harvest your own shell fish for consumption, remember to check for both PSP (and other marine toxins) and Sanitary Contamination Closures at this Fisheries and Oceans Canadawebsite - Shellfish Contamination Closures - Pacific Region (Links to an external site.)
http://www.pac.dfo-mpo.gc.ca/fm-gp/contamination/biotox/index-eng.html (Links to an external site.)
Tetrodotoxin
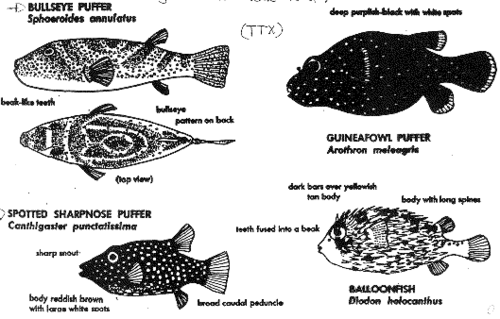
This toxin is the chemical of interest in puffer-fish or fugu poisoning. In Asian countries this hazard has been known for thousands of years. Although pufferfish have been known to be poisonous, many deaths still occur from eating these fish. Tetrodotoxin is found mainly in the ovaries, liver, intestine, skin and spawn of the various species of pufferfish. Although tetrodotoxin (TTX) was discovered in these fish, it is thought to be synthesized by a bacterial species such as Pseudoalteromonas tetraodonis associated with the puffer fish.
The meat of these fish species is considered a delicacy by the Japanese and Chinese, and the choice edible species are those that are most poisonous. The amount of poison in the fish is lowest in the summer months and increases during winter, with a peak just before spawning, in the spring.
Symptoms of pufferfish poisoning usually begin with a tingling sensation of the fingers, toes, lips and tongue a few minutes after eating the fish. Nausea, vomiting, diarrhea and epigastric pain appears in some cases. As the poisoning progresses, reflexes of the pupil and cornea are lost and the patient increasingly experiences paralysis and respiratory distress. If the dose is sufficiently large, death will result, caused by respiratory paralysis. The mode of action of tetrodotoxin is considered to be essentially the same as saxitoxin. As with saxitoxin, a lethal dose for humans is thought to be about 1.0 - 4.0 mg/kg.
Preventive measures are almost entirely restricted to diligence during preparation of the fish. When gutting and cleaning the fish, care must be exercised so as not to contaminate the flesh with even the minutest amount of viscera, ovaries or spawn.
Pufferfish poisoning continues to be a problem in Japan, affecting 30 -100 persons per year, and primarily as a result of home preparation and consumption, not from commercial sources of the pufferfish. Again we have an example of an extremely toxic chemical but one whose hazard is quite variable. Lovers of fugu are at considerable risk, while those who do not consume this food are at absolutely no risk.
| Want to learn more? |
|