The Medicalization of Childbirth

Medicalization

Medicalization is a process by which human problems come to be defined and treated as medical problems. [1] It consists of acts such as using medical language to describe a problem, adopting a medical framework to understand a problem or using a medial intervention to treat it. [1] Medicalization can be measured as a continuous value, which means a phenomenon can increase and decrease in medicalization. The decrease of medicalization is defined as demedicalization. [1]
How did medicalization start?
Traditionally, medicalization rose through doctors who had great power over people. [1] This power gave them the ability to control people’s health and society, which is termed "medical imperialism". [1] Recent analysis has shown that instead of doctors increasing medicalization, it is the pharmaceutical industry that has been pushing to invent new disease categories as a way to make more profit. [1]
Historical Overview of Childbirth in North America
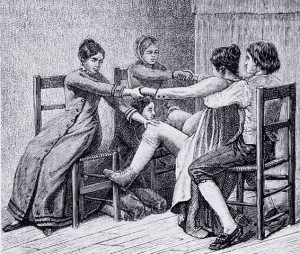
In the 20th century, most births take part in hospitals with the assistance of medical technology. A few centuries ago birth took part in the home with the help of midwives. [2] Up until the 1600s, birth was in the female exclusive arena and men were only involved when there was a difficult birthing situation. In the 1700s, doctors became involved in deliveries. [2] Having a lack of education in the subject, destructive instruments were used to deliver babies which often resulted in the death of the baby and/or the mother. [2] It was not until 1723 that forceps were introduced and this invention was the hallmark of the obstetric era. [2] Forceps are a surgical instrument shaped like a pair of tongs that were used to assist the delivery of a baby. [2] Over the years and most evidently in the 20th century in the US, doctors became highly relied on for childbirth instead of midwives. [2] Births began taking place in hospitals because of medical technology advancements and midwife use diminished. [2]
Birthing Practices in North America in the 21st Century
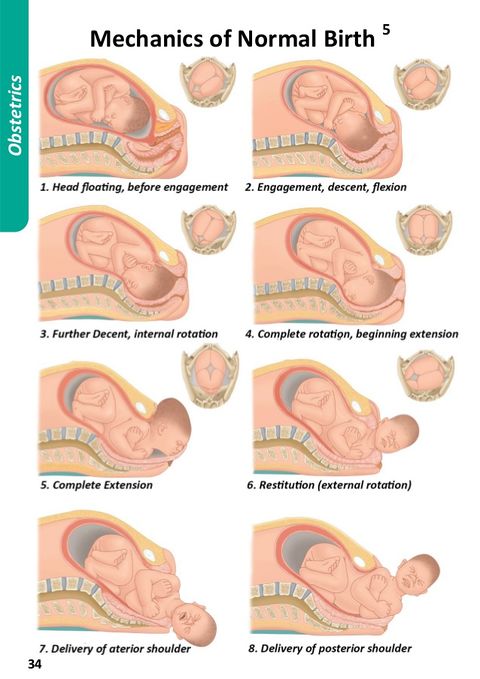
Normal Birth
What Happens in Normal (Vaginal) Birth?
A normal birth, defined by midwives and obstetricians, is a vaginal birth in which labour starts spontaneously, labour progresses without assistance or specific drugs and forceps not used.[3]The normal labour process has three stages. [3] First, the muscles of the uterus start to contract and then relax. [3] What these contractions work to do is thin and dilate the cervix to make room for the baby to pass through the birth canal. [3] Second, when the cervix is dilated completely to about 10 centimetres the baby is born. [3] Third, after the baby is born the woman will continue to have contractions until the placenta is delivered. [3]
Caesarean
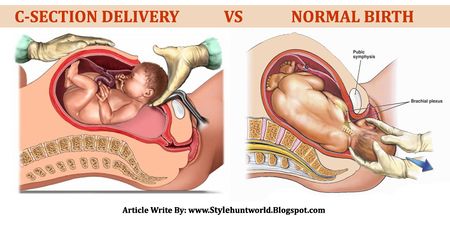
What Is a Caesarean Section?
A caesarean section, otherwise known as a c-section, is a method of childbirth where a baby is delivered through a surgical incision in the mother’s abdomen and uterus. [4] An elective caesarean section can be scheduled in advance for women who fit certain characteristics. [5] However, many times the procedure is a quick response to an unforeseen complication. [4] Many caesareans are perimorterm caesareans meaning the procedure is used to save the life of a mother and/or her baby [5]. The probability of a woman in Canada and the United States of having a caesarean section depends on her age, ethnicity, gestational age at delivery, body mass index and state during birth. [5] Caesarean sections are often considered risky as they are associated with an evident rise in severe maternal morbidity such as wound hematoma, hysterectomy, anesthesia complications, venous thromboembolism, puerperal infection and hysterectomy for hemorrhage [6].
While an elective caesarean section is a surgery that is scheduled in advance, an emergency caesarean section is one that is done urgently because of serious risks to the baby or mother during labour. [6] A growing subset of caesarean sections is the mother-request caesarean. [6] In this case, women request an elective caesarean although not meeting medical indications (not physician-suggested caesarean). [6] Characteristics of these women include fear and anxiety about birth, depression, higher maternal age, lower education, no marital status or cohabitation and certain cultural and socioeconomic views. [6]
This rise is caesarean deliveries shows to be attributed to the broadening of indications for elective Caesareans, increase in maternal request and scheduled repeat caesareans. [6] Caesarean section rates now pass 30 percent of births in many industrialized countries. [6] This is a growing concern globally because of the negative maternal and infant health outcomes. [5] The World Health Organization recommended 15% as an ideal caesarean rate and states that anything above is a sign of "inappropriate usage". [5]
This rise in caesarean deliveries shows to be attributed to the broadening of indications for elective caesareans, increase in maternal request and scheduled repeat caesareans.[6] Caesarean sections are among the most popular surgical procedures in Canada. [6] In 2012, rates in some areas of the country neared 30% of total births. [6]
In the United States, caesarean deliveries are considered the most frequent major surgery. [5] In 2009, the US rate of caesarean delivery was 32.9%. [5] To have an idea of the fast increase the caesarean delivery rate was 20.7% in 1996. Factors that have added to the increase of caesarean delivery in the US are maternal-request caesareans and repeated elective caesareans. [5] It has been suggested that maternal-request caesareans could account for 4% to 18% of caesarean births in the US. [5] The US Healthy People 2020 goals has suggested that the US take the initiative to decrease the primary caesarean rate to 23.9%. [5]
Movements to Demedicalize Childbirth
Feminist Approach
In traditional feminist literature, the medicalization of childbirth is often a topic up for critique. [7]For traditional feminists, having a ‘natural’ birth means experiencing birth without the use of medical technology where a woman is actively participating and has control over the childbirth process. [7] Even the birth setting is considered important as feminists believe that the hospital setting is a place that tempts women to use medical technologies, such as epidurals, in times of great discomfort. [7] It is suggested that the ‘natural’ route is not only a normal birth but a birth in the home with the use of midwives. [7] For natural birth advocates, it is seen that caesarean sections do not allow women control over their bodies leading to anxiety that further reduces a woman’s natural capacity for childbirth. [8] The increasing frequency of cesearean sections is seen to reflect the rise of power of masculinist medicine over women’s bodies. [8] Feminists believe maculinist medicine promotes the disempowerment and alienation of women. [8]
A Push to Reduce caesarean Sections

If the medicalization of childbirth, specifically caesarean sections, is to be reduced initiatives to reduce fear of normal childbirth have to taken by media, midwives and obstetricians. [9]In Canada, the Canadian health minister has stated that maternal and newborn programmes in Ontario have taken the initiative towards lowering caesarean section rates overtime. [6] Meanwhile in the United States, the US Healthy People 2020 goals has suggested that the US take the initiative to decrease the primary caesarean rate to 23.9%.[5] As well, the World Health Organization has suggested that caesarean rates be reduced to at most 15% to minimize inappropriate usage.[5]
Medicalization in Media


Childbirth in media, such as television shows and films, is often portrayed as a painful, hellish, and risky experience. [10] As television often overdramatizes birth to entertain viewers, television media has an effect on how childbirth is perceived by society. [10] Not only does it shape expectations of birth but it also influences women’s choices of delivery method and birth location. [10] As most births occur in a hospital setting and involve medical technology, it is argued that television portrayal of childbirth is in some part responsible for rising rates of medicalization of childbirth in the 21st century. [10]
Reference Page
- ↑ 1.0 1.1 1.2 1.3 1.4 1.5 Halfmann, D. (2012). Recognizing medicalization and demedicalization: Discourses, practices, and identities. Health, 16(2), 186-207. doi:doi: 10.1177/1363459311403947
- ↑ 2.0 2.1 2.2 2.3 2.4 2.5 2.6 Johanson, R., Newburn, M., & Macfarlane, A. (2002). Has the medicalisation of childbirth gone too far? BMJ. Retrieved from https://www.ncbi.nlm.nih.gov/pmc/articles/PMC1122835/.
- ↑ 3.0 3.1 3.2 3.3 3.4 3.5 What is a natural birth? (2015, March). Retrieved December, 2016, from http://www.babycentre.co.uk/x25016321/what-is-a-natural-birth
- ↑ 4.0 4.1 C-section: giving birth by caesarean section (2016, March). Retrieved December, 2016, from http://www.babycentre.co.uk/a160/c-section-giving-birth-by-caesarean-section
- ↑ 5.00 5.01 5.02 5.03 5.04 5.05 5.06 5.07 5.08 5.09 5.10 5.11 Dresang, L., & Leeman, L. (2012, March). Cesarean Delivery. Primary Care: Clinics in Office Practice, 39(1). Retrieved from http://www.sciencedirect.com/science/article/pii/S0095454311000947
- ↑ 6.00 6.01 6.02 6.03 6.04 6.05 6.06 6.07 6.08 6.09 6.10 Hutton, E., & Kornelsen, J. (2012, June). Patient-Initiated Elective Cesarean Section of Nulliparous Women in British Columbia, Canada. Birth Issues in Perinatal Care, 39(3). doi:10.1111/j.1523-536X.2012.00546.x
- ↑ 7.0 7.1 7.2 7.3 Behruzi, R., Hatem, M., Goulet, L., Fraser, W., & Misago, C. (2013). Understanding childbirth practices as an organizational cultural phenomenon: A conceptual framework. BMC Pregnancy and Childbirth. doi:10.1186/1471-2393-13-205
- ↑ 8.0 8.1 8.2 Malacrida, C., & Boulton, T. (2014). The best laid plans? Women’s choices, expectations and experiences in childbirth. Health, 18(1), 41-59. doi:10.1177/1363459313476964
- ↑ Brodsky, P. (2008). Where Have All the Midwives Gone? The Journal of Perinatal Education, 17(4), 48-51. doi:0.1624/105812408X324912
- ↑ 10.0 10.1 10.2 10.3 Luce, A., Cash, M., Hundley, V., Cheyne, H., Teijlingen, E., & Angell, C. (2016). “Is it realistic?” the portrayal of pregnancy and childbirth in the media. BMC Pregnancy and Childbirth. doi:DOI: 10.1186/s12884-016-0827-x