Course:MEDG550/Student Activities/Alport Syndrome
Alport syndrome is an genetic condition that is caused by changes in the Type IV Collagen genes. [1] Collagen is a scaffolding that the body uses to create structure. Changes in the genes cause an altered structure of collagen that affect the function of the kidneys, ears and eyes. The incidence of Alport syndrome is 1 in 5000 individuals, and is most commonly associated with a genetic change on the X chromosome within the collagen gene that prevents it from functioning properly. Alport Syndrome is most commonly inherited in an X-linked pattern, but has also been described to be inherited in both autosomal dominant and recessive patterns.[2]
Signs and Symptoms
Alport syndrome typically has an early onset, presenting in late childhood and early adolescence, although some inherited forms do not manifest until adulthood. The majority of affected individuals have declining kidney function (present in 90%), hearing loss (80-90%) and vision problems (20-40%). [2]
X-Linked Alport Syndrome (XLAS)
Males
Kidney (Renal) Involvement:
- Small amount of blood in the urine (hematuria)
- Kidney disease
- Protein in the urine (proteinuria)
- Formation of scar tissue in glomerulus and kidney (fibrosis)
- End-stage renal disease (ESRD); before the age of 30 [2]
Ear (Auditory) Involvement:
- Can be born with normal hearing
Eye (Ocular) Involvement: [2]
- Abnormal shaped eye lens (anterior lenticonus)
- Corneal opacities
- Flecks in the macular region (maculopathy)
- Small break in eye tissue (Macular hole)
- Retinal thinning (on OCT)
- Peripheral damage (retinopathy)
- Benign eye tumors (Leiomyomatosis)
Females[4]
Females are generally viewed as "carriers" for XLAS, yet they can also be found to express some of the same symptoms men do. Generally females expression of the symptoms are less severe and later later onset. Information about age of onset and disease severity is typically based on the individual female rather than family history.[2][4]
| Small amount of blood in the urine (Hematuria) | At least 95% |
| Protein in the urine (Proteinuria) | Common from early adulthood |
| Kidney Disease | Prevalence and age not known |
| ESRD | 15%–30% by the age of 60 yr |
| Hearing loss | Later Onset; Common from middle age |
| Corneal opacities | Often undetected, occurs even with normal renal function |
| Abnormal shaped eye lens (Lenticonus) | Very Uncommon |
| Central fleck damage (maculopathy) | 30% |
| Retinal thinning (on OCT) | 50% of hospital-based females |
| Small break in eye tissue (Macular hole) | Uncommon; but occurs |
| Peripheral damage (retinopathy) | 50% |
| Benign eye tumors (Leiomyomatosis) | Uncommon |
- Savige, J., Colville, D., Rheault, M., Gear, S., Lennon, R., Lagas, S., . . . Flinter, F. (2016). Alport syndrome in women and girls. Clinical Journal of the American Society of Nephrology : CJASN, 11(9), 1713-1720. doi:10.2215/CJN.00580116
Autosomal Recessive Alport Syndrome (ARAS)
People that are carriers of ARAS only have one altered copy of the gene and are not expected to present with symptoms.[1] [2]
Autosomal Dominant Alport Syndrome (ADAS)
Autosomal Dominant Alport Syndrome has the least severe symptoms of the Alport Syndrome types. Previously, ADAS went undetected, undiagnosed or mis-diagnosed (as Thin Basement Membrane Disease). Now that more is known about ADAS, it is seen in about 1% of the population [5].
Persons with ADAS will have a gene change in COL4A3 or COL4A4. They often have protein in their urine, which will look like foamy urine and blood in urine. Blood in urine may not happen every time your urinate.
More rare symptoms of ADAS are: hearing loss that can happen in later adulthood, end-stage kidney failure in later adulthood. Very rarely are there there any symptoms of ADAS that affect a persons eyes. [6]
Cause
Alport syndrome is an genetic disorder that is caused by changes in the Type IV Collagen genes. [1] Genetic conditions are caused by changes in our DNA that can be passed from generation to generation. DNA is a long string of letters (A, T, G, and C) whose sequences determines instructions cells use to carry out functions. Each function is attributed to a gene. Alport syndrome genes code for Type IV Collagen.
Collagen and other glycoproteins make up the basement membrane; this layer provides structural support to the tissues within the body. [7] Changes in genes that encode collagen cause a disruption of the organization of these layers, resulting in an altered structure and function of the kidneys, ears and eyes.
The normally functioning forms of these genes produce three different chains (-chains) of type IV collagen, which interact in groups of three. When faulty -chains are produced the chains are unable to interact properly and lead to the weakness of the basement membrane. [7]
Diagnosis
Alport syndrome is diagnosed by: [8]
- A complete family history taken by a medical doctor or genetic counsellor:
- Identify any affected individuals.
- Determine the severity of disease in the family
- Determine age of onset
- Presence of kidney disease, deafness, blindness, and high blood pressure
- Complete physical exam, blood electrolytes and urinalysis
- Referrals for hearing specialist (audiology) and eye doctor (ophthalmology).
- Biochemical or molecular testing for COL4A5, COL4A3, and/or COL4A4 gene sequences
- Skin biopsy staining for the type IV 5-chain
- RT-PCR
- Exome sequencing of COL4A5,COL4A3, and/or COL4A4
Prevalence
The prevalence of Alport syndrome in the general population is around 1 in 5 000 in the U.S., and the autosomal recessive Alport syndrome is estimated to affect 1 in 50 000[9] [4] The incidence of Alport Syndrome was found to be substantially lower in Finland effecting 1 in 53 000, and Souther Sweden at 1 in 17 000.[9] Alport is seen in twice as many females as males; this is because the majority of Alport is X-linked where men can only pass the condition on to their female children and not to their male children.[4]
Management and Treatment
Kidneys
Once identified, kidney function is continually assessed. In addition, individuals with Alport syndrome are often monitored and treated for high blood pressure, or hypertension, because of the potential impact on blood pressure due to its relationship with kidney function. [1]
Treatment involves the use of angiotensin converting enzymes (ACE) inhibitors, as these have been shown to be highly effective in children, with minimal side effects. [1] As the disease progresses, dialysis is used to help the body by filtering the blood through an external filtration system and kidney transplantation is considered.
Ears
Ongoing hearing assessments are used to detect progression and hearing aids are prescribed as needed.[2]
Eyes
Detailed and regular ophthalmological appointments are used to monitor progression and provide surgical interventions when needed.[2]
Women Carriers of XLAS
Should be tested annually for albuminuria and hypertension.[4]
Inheritance Patterns
Alport syndrome is caused by mutations in type IV collagen genes (COL4A5, COL4A3, COL4A4 ), and can be inherited in three different patterns: X-linked, autosomal recessive or autosomal dominant.[2]
Most Common - X-Linked
X-Linked Alport Syndrome (XLAS) is caused by mutations in the COL4A5 gene located on the X chromosome and accounts for approximately two-third of all Alport's Syndrome cases[6]. [1]As an X-linked condition, males typically have a more severe presentation than females, as males only have one X chromosome. In females, the presence of a functional gene on the second X chromosome can partially compensate for the mutated gene on the opposite X chromosome, but males do not have this compensatory effect.
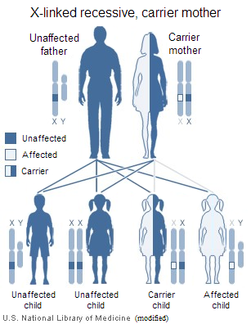
Carrier Mother
A mother who is a carrier for XLAS has one affected X chromosome, and one unaffected X chromosome. and can pass down the affected X chromosome to either a son or a daughter. Both affected sons and carrier daughters would have a risk of an affected future child.
Chance of Having an:
- Affected male is 50%
- Unaffected male is 50%
- Carrier female is 50%
- Non-carrier female is 50%
Affected Father
A father affected with XLAS has one affected X chromosome, and one unaffected Y chromosome. The father can only pass the affected X chromosome to his daughters and the unaffected Y to his sons. The daughter will be a obligatory carriers of XLAS and would have future risk for her children. The sons will not be carriers of XLAS and there is no further risk to the sons future children.
Chance of Having an:
- Affected male is ~ 0%
- Unaffected male is 100%
- Carrier female is 100%
- Non-carrier female is ~ 0%
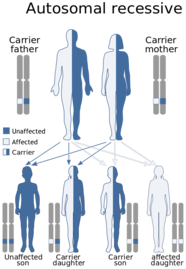
Autosomal Recessive
Mutations in either COL4A3 or COL4A4 are responsible for autosomal recessive (ARAS). ARAS accounts for ~15% of all Alport Syndrome cases [6] The term recessive means that both copies one form mom and one from dad need to be affected to display ARAS.
Because in ARAS both the mom and dad are carriers there is a 25% chance that they will have a child affected with ARAS, a 50% chance that they will have an unaffected child who is a carrier, and a 25% chance that they will have a child who carries no mutated copies of the gene.
There is no difference in risk between male and female children.
Autosomal Dominant
Mutations in either COL4A3 or COL4A4 are responsible for autosomal dominant (ADAS) Alport syndrome. ADAS now accounts for 20% of all Alport's Syndrome cases[6]. The term dominant means that only one gene change from mom or from dad is needed to ADAS.
Because in ADAS an individual only needs one of their two gene copies affected, there is a 50% chance to pass on the unaffected gene, and have an unaffected child or a 50% chance to pass on the affected gene and having an affected child.
There is no difference in risk between male and female children.
Genetic Counselling
Genetic counselling helps individuals and families understand and adapt to the implications of genetic testing.[10] In the context of Alport syndrome, it involves:
- Collecting a detailed family history. This helps identifying the inheritance pattern, and risk for other family members. It will also provide information about how the disease might progress in the family.
- Reviewing information about the disease. This includes a discussion about genes, chromosomes and inheritance patterns.
- Providing risk estimates. Individuals, or couples, who know of the disease in their families may see a genetic counsellor to find out the chance of having an affected child, or a child who is a carrier. Women who are already pregnant may want information about prenatal testing options.
- Helping to facilitate genetic testing. If patient is undiagnosed the use of genetic testing can help to provide a definitive diagnosis through identification of affected COL4A5, COL4A3, COL4A4 genes.
- Supporting the individuals, couples and families as they make decisions about testing. This includes helping individuals, couples and families respond to a diagnosis, or test result.
Helpful Resources
Canada specific: http://www.alportsyndrome.ca/
Australia specific:http://www.alport.org.au/HOME.html
Germany specific: http://www.alport-selbsthilfe.de/
- John F. Martin Website - A photojournalist's website who was diagnosed with Alport’s syndrome. The site chronicles the journey through dialysis and transplant. The site contains many graphic photos of medical procedures, may not be suitable for younger children
- Kidney Steps - A 5-step program to with helpful advice for surviving kidney disease
- Facebook page for USA-based support group
References
- ↑ 1.0 1.1 1.2 1.3 1.4 1.5 Kashtan, C., Ding, J., Gregory, M., Gross, O., Heidet, L., Knebelmann, B.,…Licht, C. (2013) Clinical practice recommendations for the treatment of Alport syndrome: A statement of the Alport Syndrome Research Collaborative. Pediatric Nephrology, 28(1), 5-11.
- ↑ 2.0 2.1 2.2 2.3 2.4 2.5 2.6 2.7 2.8 2.9 Kashtan CE. Alport Syndrome and Thin Basement Membrane Nephropathy. 2001 Aug 28 [Updated 2013 Feb 28]. In: Pagon RA, Bird TD, Dolan CR, et al., editors. GeneReviews™ [Internet]. Seattle (WA): University of Washington, Seattle; 1993-. Available from: http://www.ncbi.nlm.nih.gov/books/NBK1207/
- ↑ Merchant SN, Burgess BJ, Adams JC, Kashtan CE, Gregory MC, Santi PA, Colvin R, Collins B,... Nadol JB. Temporal bone histopathology in alport syndrome. Laryngoscope. 2004;114:1609–18.
- ↑ 4.0 4.1 4.2 4.3 4.4 Savige, J; Colville, D; Rheault, M; Gear, S; Lennon, R; Lagas, S; Finlay, M; Flinter, F (September 2016). "Alport Syndrome in Women and Girls". Clinical Journal of the American Society of Nephrology. 11 (9): 1713–1720.
- ↑ Savige, Judy (2024-01-26 17:15:42). "Heterozygous Pathogenic COL4A3 and COL4A4 Variants (Autosomal Dominant Alport Syndrome) Are Common, and Not Typically Associated With End-Stage Kidney Failure, Hearing Loss, or Ocular Abnormalities". Kidney International Reports (published 09/2022). 7: 1933–1938. doi:10.1016/j.ekir.2022.06.001. Check date values in:
|date=, |publication-date=(help) - ↑ 6.0 6.1 6.2 6.3 https://www.ncbi.nlm.nih.gov/books/NBK1207/. Missing or empty
|title=(help) - ↑ 7.0 7.1 LeBleu, V., Macdonald, B., Kalluri, R (2007). Structure and function of basement membranes. Experimental Biology and Medicine, 232 (9), 1121-1129.
- ↑ Hertz, J., Thomassen, M., Storey, H., Flinter, F. (2012) Clinical utility gene card for: Alport syndrome. European Journal of Human Genetics, 20(6), doi:10.1038/ejhg.2011.237.
- ↑ 9.0 9.1 Hertz, J; Thomassen, M; Storey, H; Flinter, F (2012). "Clinical utility gene card for: Alport syndrome". European Journal of Human Genetics. 20(6): 713–713.
- ↑ Resta, R., Biesecker, B., Bennett, R., Blum, S., Hahn, S., Strecker, M., Williams, J. (2006). A new definition of genetic counseling: National Society of Genetic Counselors’ task force report . Journal of Genetic Counseling, 15(2), 77-83.